What Is
Verrucae needling or otherwise known as Falknor’s needling is an innovative and effective procedure for eradicating benign types of Human Papillomavirus (HPV). The aim is to break down the verrucae, pushing it to the deeper layers of the skin causing a controlled inflammatory response. This stimulates the body’s immune system to recognise and destroy the virus.
This type of soft tissue therapy has been around for over 45 years, first being described in a medical journal in America in 1969. It is commonly carried out internationally by many practitioners and has been reported to be highly effective, even for long-standing verrucae.
Falknor’s needling is the more preferential option compared to the usual cryotherapy and acid treatments available, as it frequently only requires a single treatment. This makes it a more practical and desirable treatment option for the busy person who cannot come in for regular appointments.
How Does It Work?
Puncturing the viral verruca/wart with a sterile needle many times causes the viral particles to become exposed to the deeper layers of the skin and the fatty tissue beneath, where there is vast blood circulation.
The immune regulators in the blood recognise the presence of the viral infection and mediate an attack to destroy the virus. As this immune response is often systemic, treatment of only one verruca is required, even when there are many lesions, a spontaneous remission can occur in all, or most, verrucae at the same time.
What Does Falknor's Needling Involve?
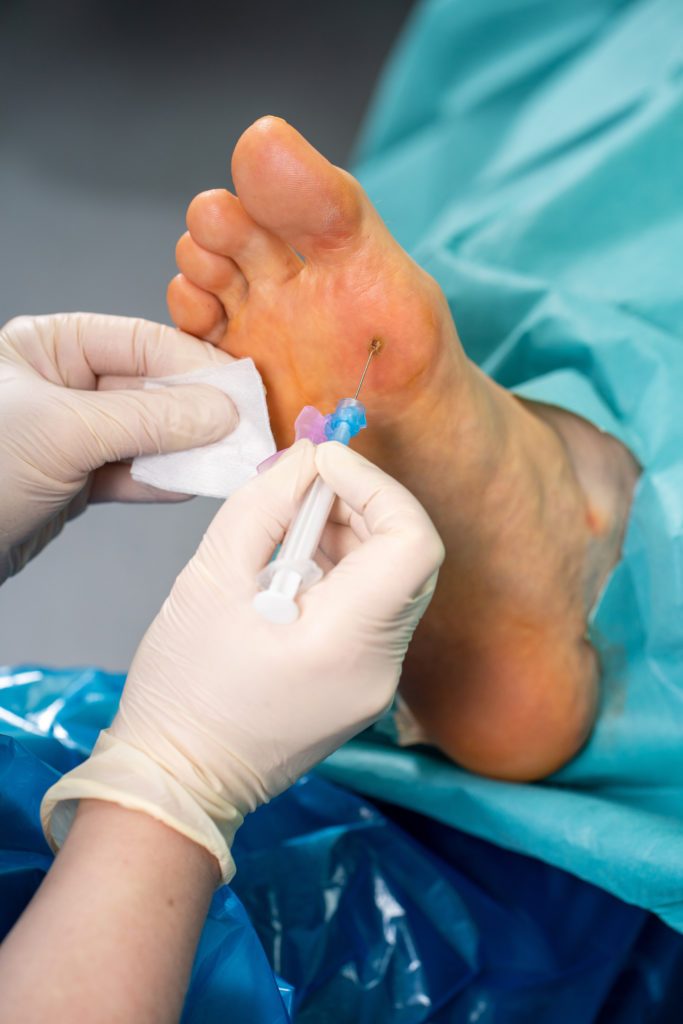
1. A local anaesthetic will be administered to anaesthetise the area being treated making the surrounding area numb.
2. Once the area is anaesthetised the area will be reduced to remove any overlying callus if necessary.
3. The podiatrist will carefully needle the verrucae to push the virus to the deeper layers of the skin, so that the body’s immune system can come into contact with the virus.
4. A dressing will be applied once the treatment is complete and the podiatrist will provide you with aftercare advice.
Will it be painful?
The anesethetic administered should provide pain relief for a few hours post treatment. Patients can experience a little tenderness and soreness in the area after the anaesthetic wears off, feeling like the area has been bruised for 1 to 2 days. We advise to take painkillers such as paracetamol to help ease the discomfort which is usually more than adequate.
Risks & Complications
Although very rare, the following risks have been noted:
● Infection
● Recurrence
● Delayed healing
● Adverse reaction to local anaesthesia
● Scar tissue